The human body is an amazing thing. For each one of us, it’s the most intimate object we know. And yet most of us don’t know enough about it: its features, functions, quirks, and mysteries. Our series The Body explores human anatomy part by part. Think of it as a mini digital encyclopedia with a dose of wow.
1. IT'S SHAPED LIKE A SHOE.
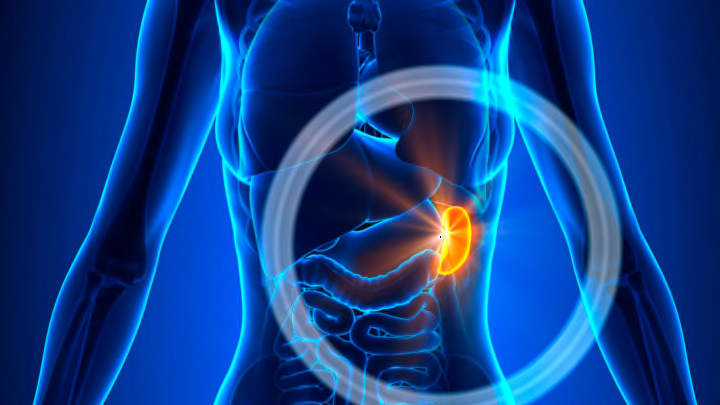
The spleen is shoe-shaped, and it’s the largest organ in the lymphatic system at a whopping 5 inches, weighing as much as 6 ounces. The organ is situated between the fundus of the stomach and the diaphragm, and connected by one little ligament to your left kidney, too.
2. IT'S A BLOOD FILTER.
Your spleen is in charge of filtering blood as it moves through your body to control the production of red blood cells. It also defines the donut-like shape of red blood cells, which must squeeze through an opening in the spleen known as the interendothelial slit. This reshapes the cells before they pass back into the blood stream—or, if they are old, misshapen, or diseased, blocks them from returning.
3. IT'S A POWERHOUSE INFECTION FIGHTER.
As recently as 2009, researchers discovered that the spleen plays host to a special cache of immune cells called monocytes. If the human body suffers a serious trauma, such as a heart attack, wound, or big infection, the spleen sends those monocytes into the blood stream to fight off infection.
4. ITS LOCATION IS BOTH IDEAL AND DANGEROUS.
From Anatomy of the Human Body by Henry Gray via Wikimedia Commons // Public Domain
The spleen is neatly tucked up under the left side of the rib cage, where it’s protected by those lateral bones. But this also means a broken rib could pierce the fragile organ and rupture it. If the organ is breached, usually during a traumatic injury like a car accident, it has to be removed immediately. Because the spleen has so many blood vessels, a person would otherwise bleed to death.
5. YOU CAN LIVE WITHOUT IT.
Unlike, say, your stomach or lungs, the spleen is not considered a “vital” organ, which simply means that it can be surgically removed and you’ll be mostly fine, though potentially prone to more infections.
6. THERE HAVE BEEN SPLEEN TRANSPLANTS.
A handful of these procedures have been done with some success on humans to boost infection-fighting power, but they are rare, and are usually transplanted in patients who have already lost their own spleens.
7. NO ONE LIKES A SPLEENFUL PERSON.
In medieval times, people believed your spleen was the source of “morose feelings and bad temper.” The connotation entered into common speech (via Latin, splen)—no one would want to be around you if you were spleenful, though spleenless was a prized way to be. Today, the word spleen is still in Webster’s Dictionary meaning “feelings of ill-will or anger, often suppressed.”