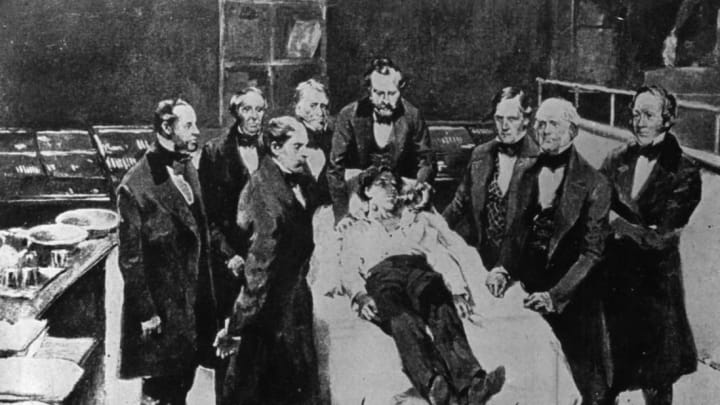
16th October 1846: Doctors at Massachusetts General Hospital re-enact the first ever use of medical anesthetics.
In 1800, Lord Thurlow, a member of British Parliament, stated “There is no more science in surgery than in butchering." Surgeries, such as amputations and mastectomies, were painful, brutal, quick, crude, loud (imagine all of the screaming patients), and dangerous. In the 1830s, 30 to 50 percent of patients died during amputations, a fact that contributed to the prevailing attitude that surgeons were barbaric and unskilled.
The distinction between doctors and surgeons originates in the 5th century BCE. The Hippocratic Oath distinguished physicians from craftsmen who worked with their hands and were equipped to “use the knife,” and even the modern version distinguishes the roles. In 18th century Britain, medical schools viewed surgery as a manual rather than intellectual craft, so barber-surgeons did not need a university education like the higher status gentlemen-physicians did. America, however, was less rigidly stratified than Europe and considered everyone who practiced medicine to be a doctor, partly due to the lack of medical schools.
In France, they split barber-surgeons from barber-wigmakers in 1717, but both remained primarily barbers. In 1756 the French effectively separated surgeons from barbers by requiring a master of arts degree for surgeons (though this law was only enforced in large cities). This was spurred along by the founding in 1750 of a College of Surgery. After the revolution occurred, however, the number of doctors plummeted. In 1793, there were 2,700 “health officers” in the French army, but by 1794 they’d lost almost a thousand of them. And there were concerns that what doctors remained were undereducated. This led to a push for unification of doctors and surgeons in France.
In the early 1800s, medical schools in France began encouraging doctors to focus on specific organs, detailed observation of patients, and autopsy. This period, known as Paris Medicine or Hospital Medicine, set the stage for an increased reliance on surgery because doctors were honing in on specific body parts rather than taking a more holistic, broad approach to treating patients. A few decades later, during the 1820s to 1850s, America experienced a Paris Period in which American physicians traveled to Paris to study these ideas.
However, what really cemented the dramatic rise in status for surgeons—from under-educated, unskilled barbarians to respected, highly paid doctors—was the development of anesthesia. Anesthesia’s first medical use in 1846 was a game changer, paving the way for medicine to become more safe, effective, and reliable. On October 16, 1846, dentist William Morton gave the first public demonstration of ether at Boston’s Massachusetts General Hospital. While he anesthetized the patient, a surgeon removed the patient’s tumor successfully, and Morton proved that anesthesia was safe and effective.
Within months, surgeons in both America and Europe began using anesthesia routinely. Consequently, surgeons were now free to work more slowly, carefully, and precisely with good asepsis. Rather than amputating a patient’s leg as quickly as possible to minimize his or her excruciating pain, surgeons could work methodically and deliberately, free from the distraction of a screaming patient. A newfound respect for surgeons arose since surgical operations became controlled, professional environments rather than struggles to physically restrain patients writhing in agony.
As doctors gave support for ether as a safe and effective anesthetic, surgeons gained credibility and respect in the eyes of the public. In 1877, deaths due to ether were 1 in 23,204, making ether about eight times safer than chloroform (1 death per 2,873). Additionally, more medical schools for surgeons and increased regulation of the profession contributed to the public’s perception of surgeons as legitimate, reliable, trustworthy physicians working in their own special sphere of medicine. And that's why no one goes to their surgeon for a shave and a haircut anymore.