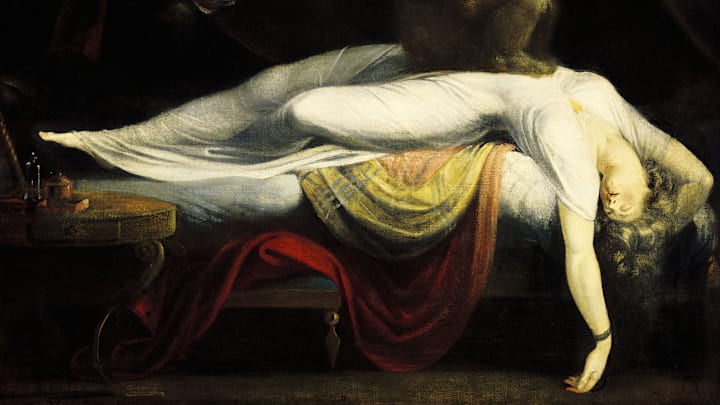
Before “that time of the month” became a catch-all excuse for a woman’s mood swings, there was another, stranger uterus-adjacent reason for female distress: hysteria. This wasn’t just a misogynistic saying—it was once a legitimate medical diagnosis. Today, the word is mostly shorthand for rage, sadness, or frustration, but for centuries, hysteria was seen as an actual condition. Historically, there haven’t been many things women had that men didn’t—from ballots to basic autonomy—but a hysteria diagnosis was one thing that decidedly favored women over men…unfortunately.
The Wandering Womb
Half-bull monsters and snake-haired gorgons weren’t the most far-fetched of Greek myths. The wildest one might have been entirely human: the idea that a wandering womb could wreak havoc on the body. From ancient Greek physicians like Hippocrates to Victorian-era doctors, this bizarre belief held that the uterus could move through the body, causing everything from fainting and paralysis to grief and rage.
The term hysteria comes from the Greek hystera, meaning womb, and because the myth revolved around female anatomy, only women were considered susceptible. Treatments were just as strange as the idea itself: aromatic therapies, induced sneezing, or even sex and marriage were prescribed to coax the uterus back into place.
Beneath the curious cures lay a darker truth: the wandering womb myth reflected a broader societal belief that women were emotionally unstable and physically fragile, and that their bodies could be blamed for nearly any misfortune. Virtually any symptom—from fevers to kleptomania—could be chalked up to a restless uterus.
Centuries later, this myth would leave the textbooks and hit the stage—literally—when Victorian women fainted, contorted, and performed hysteria for doctors at Paris’s famed La Salpêtrière Hospital.
Faints, Fits, and Fascination
Paris in the 19th century was a city of spectacle, from glittering ballet halls to smoky cabarets. But one of its most unusual attractions took place under hospital lights. At the Pitié-Salpêtrière, famed neurologist Jean-Martin Charcot staged weekly “hysteria shows,” transforming medical lectures into theatrical events in which female patients diagnosed with hysteria became the main attraction.
What were billed as scientific demonstrations often resembled theater. During the 1870s and 1880s, crowds of students, visiting physicians, and curious members of high society gathered as Charcot hypnotized patients and guided them into dramatic poses—arching backs, rigid limbs, sudden collapses—presented as textbook stages of hysteria. He earned the nickname “the Napoleon of neuroses,” a testament to both his authority and his flair.
The setting only amplified the drama. The demonstrations took place at Pitié-Salpêtrière Hospital, an institution that had long housed society’s most marginalized women, including the poor, the mentally ill, and sex workers. Under bright lights and the scrutiny of an audience, female patients were photographed, cataloged, and studied—images that circulated widely and helped cement hysteria as both a medical diagnosis and a cultural fascination.
But one of Charcot’s most famous students would ultimately challenge him. Sigmund Freud rejected the idea that hysteria was simply a neurological defect. Instead, he proposed that its origins lay in the psyche, a radical shift that would move hysteria from the body to the mind.
Mind Over Madness
Freud took what he saw at La Salpêtrière and added a new layer: psychology. Where Charcot blamed nerves and heredity, Freud argued that hysteria emerged from the mind—from repressed emotions, unresolved trauma, and unconscious conflict. Physical symptoms like fainting, paralysis, or dramatic fits weren’t evidence of a defective nervous system; they were signs of internal psychological struggles.
He also labeled hysteria as distinctly feminine, tied to societal pressures and sexual repression. Treatments, unsurprisingly, were still shaped by gendered assumptions. Marriage and sexual activity were recommended, echoing centuries of prior medical advice. Some historical accounts claim uterine massages were sometimes aided by early vibrators, though that’s now considered likely a myth. Either way, the treatments were meant to relieve symptoms, with little acknowledgment of their sexual undertones.
Freud turned hysteria from a medical spectacle into a psychological case study, but bias stuck around. Women were still the main subjects, and behaviors tolerated in men were often treated as symptoms in women. Even so, this shift laid the groundwork for modern psychiatry—and proved you can change the theory without changing the stereotypes.
When Misdiagnosis Meets Misogyny
After centuries of wandering wombs, medical melodrama, and Freudian claims, hysteria was officially removed from the Diagnostic and Statistical Manual of Mental Disorders (DSM) in 1980. Doctors finally confirmed what many suspected: most "symptoms" were actual mental illnesses or simply normal behaviors that society disliked in women.
Yet its shadow lingers to this day. While hysteria is gone from official diagnoses, calling someone “hysterical” still carries centuries of baggage—a synonym for emotional, angry, or “difficult” behavior, usually aimed at women. Thus, hysteria’s story isn’t just medical history; it’s a cautionary tale about how cultural assumptions about gender can shape science, medicine, and language, leaving traces long after the diagnosis disappears.